- “Empowering Emergency Medicine Physicians”
- “Queue Management Software and Hospitalists in Modern Healthcare”
- “Enhancing-Pediatric-Infectious-Disease-Care”
- “Revolutionizing-Geriatric-Care”
- “Optimizing-Patient-Care-in-Pediatric-Rheumatology”
- “Pediatric-Pulmonology-Care”
- “Revolutionizing-Pediatric-Gastroenterology”
- “Enhancing-Pediatric-Neurology-Care”
- “Optimizing-Pediatric-Cardiology”
- “Enhancing-Pediatric-Endocrinology-Care”
- “Empowering-Neonatologists-with-EMR-Software”
- “Pediatrics-in-Focus”
- “Empowering-Neurologists-with-Electronic-Prescriptions”
- “Streamlining-Dermatology-Practice”
- “Streamlining-Psychiatry-Practice”
- “A-Game-Changer-for-Infectious-Disease-Specialists”
- “Allergist/Immunologist-Practices-with-QME-EMR-and-Hospital-Management-Systems”
- “Empowering-Hematologists-and-Revolutionizing-Healthcare-Management”
- “Optimizing-Healthcare-with-HMIS”
- “Transforming-Healthcare-with-Endocrinologist”
- “Healthcare-Management-with-QMe-EMR-for-Nephrologists”
- “Revolutionizing-Healthcare-Management-with-Cardiologist”
- “Streamlining-Operations-with-Queue-Management-Software”
- “Optimizing-Healthcare-Delivery”
- “Transforming-Healthcare-Management”
- HMIS And Decision Support Systems
- Dengue Unveiled: An Overview of Causes, Symptoms, and Prevention.
- Dengue Fever: Unraveling the Mosquito-Borne Menace.
- HMIS-and-Continuity-of-Care
- Project-Management-for-Successful-HMIS
- Catalysts of Wellness: The Transformative Power of Diagnosis and Screening in Healthcare
- Patient-Data-Management
- Guardians of Healthcare: The Vital Role of Fraud Detection in Ensuring Ethical Care
- Unlocking Insights
- Healthcare in the Digital Age: The History Of Development Of HMIS
- Transforming Healthcare
- Safeguarding-HMIS-Data
- HMIS-Integration-Challenges
- ANXIETY UNVEILED: CONQUERING FEARS AND CULTIVATING CALM.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- HMIS and Resource Allocation
- HMIS Data Accuracy and Integrity
- SOOTHING THE SILENT PAIN: UNDERSTANDING VULVODYNIA.
- Impact of HMIS on OPD Operations
- In Patient Management Through Health Management
- WITHIN THE SHADOWS: UNDERSTANDING BRAIN TUMOURS FROM WITHIN
- HMIS-and-Health-Insurance-Integration
- HMIS-Data-Analytics-for-Preventive-Care
- SILENT INTRUDERS: UNRAVELLING THE MYSTERIES OF PELVIC INFLAMMATORY DISEASE
- BREAKING FREE: OVERCOMING THE HURDLE OF URINARY INCONTINENCE
- “HMIS and Doctor-Patient Communication”
- HEALING INSIGHTS: THE POWER OF THE HOSPITAL MANAGEMENT INFORMATION SYSTEM.
- SOLVING THE OVARIAN PUZZLE:UNDERSTANDING OVARIAN CYST INSIDE OUT
- Usability And User Experience In HMIS
- WARRIOR’S BATTLE: TRIUMPHING OVER UTERINE CANCER
- POLYCYSTIC OVARY PUZZLE: UNRAVELLING THE ENIGMA OF PCOS
- Unlocking-the-Potential-of-HMIS-Data-for Medical-Research-and-Healthcare-Policy-Enhancement
- Feminine Health Unplugged: Empowering Women in Vaginal Infection Awareness
- Revitalizing Feminine Comfort: A Journey Through Vaginal Wellness.
- HMIS Vendor Selection Guide
- UNDERSTANDING FIBROIDS: NAVIGATING THE INTRICACIES OF UTERINE HEALTH.
- Best Practices for Data Migration in Healthcare Management Information Systems (HMIS)
- CONCEIVING HOPE: NAVIGATING THE JOURNEY OF INFERTILITY
- MENSTRUAL IRREGULARITIES: CAUSES AND TREATMENT
- RISING ABOVE: EMPOWERING WOMEN WITH PELVIC ORGAN PROLAPSE
- Leveraging HMIS for Enhanced Public Health Management and Disease Surveillance
- Challenges and Benefits of Implementing HMIS in Rural and Remote Healthcare Settings
- Securing Healthcare Continuity
- Pancreatic Cancer
- Lymphoma
- Leukemia
- Bladder Cancer
- Skin Cancer (Melanoma)
- COLORECTAL CANCER
- All about Prostate Cancer
- Advances in Breast Cancer Treatment: A Comprehensive Guide
- Autism Spectrum Disorder (ASD)
- EHR SYMPHONY: HARMONIZING HEALTHCARE THROUGH ELECTRONIC RECORDS .
- Understanding Testicular Cancer: Detection, Treatment And Awareness.
- Childhood Obesity
- Kawasaki Disease
- Eczema (Atopic Dermatitis)
- Understanding Bone Cancer: A Brief Overview.
- Virtual Healing: Navigating Healthcare Through Telemedicine and Telehealth.
- Attention-Deficit/Hyperactivity Disorder (ADHD)
- PELVIC PAIN:CAUSES SYMPTOMS AND PREVENTIONS
- Type 1 Diabetes: Causes, Symptoms, and Treatment
- Gastroesophageal Reflux Disease (GERD)
- Battling Pneumonia: Unveiling the Stealthy Invader of the Lungs
- Unravelling the Complexity of Allergic Reactions: Understanding, Managing, and Thriving
- Rashes (Eczema, Dermatitis)
- UNDERSTANDING CERVICAL DYSPLASIA: CAUSES, SYMPTOMS AND MANAGEMENT
- Chicken Pox
- Endometriosis Unmasked: A Closer Look at the Silent Struggle
- Croup
- Hand, Foot and Mouth Disease (HFMD)
- THE DAWNING OF A NEW ERA: EMBRACING THE JOURNEY OF MENOPAUSE
- Urinary Tract Infections (UTIs)
- Strep Throat (Streptococcal Pharyngitis)
- Understanding Otitis Media(Ear Infection)
- 28th July In medical history!!
- Influenza (Flu) - Symptoms, Prevention and Management
- 27th July In medical history!!
- Respiratory Syncytial Virus (RSV) Infection
- SIGNIFICANCE AND ADVANTAGES OF HMIS: A DETAILED ANALYSIS
- Beyond Boundaries: Transforming Healthcare with Virtual Reality
- TRACK YOUR LIFE : A DETAILED UNDERSTANDING ON HEALTH MONITORING SYSTEM
- EXPLORING BENEATH THE SURFACE: UNDERSTANDING BARTHOLIN CYSTS AND ABSCESSES
- GUARDING GUT HEALTH: YOUR GUIDE TO POTENTIAL CROHN’S DISEASE PREVENTION.
- PATHWAYS OF HOPE: NAVIGATING THE CHALLENGES OF ESOPHAGEAL CANCER
- Gastric Battles: Confronting Stomach Cancer Head-On.
- HMIS IN SMALL CLINICS: A STEP TO A BETTER FUTURE
- Harmonizing Your Cycle: A Journey to Menstrual Health and Balance.
- Respiratory Syncytial Virus (RSV) Infection
- GUARDING OUR INTIMATE WORLD: A CLOSER LOOK AT STI
- Real-World HMIS Implementation Case Studies: Using Data to Transform Healthcare
- Gastroenteritis (Stomach Flu)
- Asthama - The Anatomy Of Breathing
- Influenza - A Silent Intruder
- Breast Cancer
Fighting out the Disease of Lung Cancer
Fighting out the Disease of Lung Cancer
Lung Cancer
Lung cancer, a devastating healthcare concern, stands as one of the most prevalent and life-threatening malignancies globally. This illness begins in the lung tissues and is frequently brought on by a combination of genetic predispositions, environmental exposures, and most importantly, cigarette use. Lung cancer has a significant impact on healthcare systems due to its many subtypes, including non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC). Although early detection and improvements in treatment have improved results, handling late-stage cases still presents difficulties. To lessen the significant health and financial consequences of lung cancer, healthcare systems around the world must address its complications.
Types and Subtypes of Lung Cancer
Non-Small Cell Lung Cancer (NSCLC)
1. Adenocarcinoma
The glandular cells that line the airways of the lung are where the common kind of lung cancer known as adenocarcinoma develops. It frequently affects non-smokers and manifests subtly, delaying diagnosis. Effective therapy depends on early discovery. The various molecular profiles of adenocarcinomas have opened the door for tailored medicines, changing the treatment of lung cancer.
2. Squamous cell carcinoma
Squamous cell carcinoma, another lung cancer variant, develops in the flat cells lining the lung’s inner airways. Typically associated with smoking, it tends to cause symptoms like chronic cough and wheezing. Early diagnosis is essential for favorable outcomes. While advancements in treatment have improved prognosis, challenges persist due to late-stage diagnoses. In order to treat this aggressive form of lung cancer, a multidisciplinary strategy comprising surgery, chemotherapy, radiation therapy, and cutting-edge targeted therapies is essential.
3. Large cell carcinoma
Non-small cell lung cancer of the large cell variety is distinguished by its aggressive and quick-growing nature. These cancer cells are difficult to categorize into particular subgroups since they appear big and aberrant under the microscope. Due to its aggressive behavior, early diagnosis and prompt intervention are vital. For the best results, treatment usually entails a mix of surgery, chemotherapy, and radiation therapy that is specifically adapted to the patient’s situation.
Small Cell Lung Cancer (SCLC)
An aggressive type of lung cancer known as small cell lung cancer (SCLC) is well known for its quick development, ability to spread, and close connection to smoking. This neuroendocrine tumor often originates in the bronchi and can swiftly metastasize to distant organs. Characterized by its small cell size and tendency to respond initially to chemotherapy and radiation, SCLC eventually develops resistance, leading to challenges in long-term management. Combining systemic healthcare treatments with radiation and immunotherapies has the potential to improve the quality of life and extend survival for SCLC patients.
Rare and Emerging Subtypes
1. Carcinoid tumors
Carcinoid tumors, uncommon lung cancers originating from neuroendocrine cells, exhibit a relatively indolent growth pattern. These tumors have the capacity to release hormones and bioactive compounds, which might result in symptoms including flushing and diarrhea. Surgical removal is often curative for localized cases. Treatments for advanced or metastatic carcinoid tumors may need to target hormone synthesis and receptor pathways. Although they tend to grow more slowly than other types of lung cancer, the variety of their presentations emphasizes the need for tailored care strategies.
2. Pleomorphic carcinoma
Pleomorphic carcinoma, a subtype of non-small cell lung cancer, is characterized by its mixed histological composition and aggressive behavior. It presents diagnostic difficulties because it is heterogeneous and contains several cell types. Frequently diagnosed at an advanced stage, treatment involves a combination of surgery, chemotherapy, and radiation therapy. Despite its rarity, it is essential to comprehend the distinctive aspects of pleomorphic carcinoma in order to develop successful therapeutic approaches adapted to its particular traits.
3. Others
Among other rare lung cancer subtypes are sarcomatoid carcinoma, which displays both carcinomatous and sarcomatous components, and mucoepidermoid carcinoma, typically originating in the salivary glands but occasionally found in the lungs. These subgroups highlight how diverse lung cancer is, calling for specialist diagnostic methods and therapeutic strategies. Research into these rare variants has the potential to shed new light on the biology of lung cancer and improve therapeutic approaches for better patient outcomes.
Causes and Risk Factors
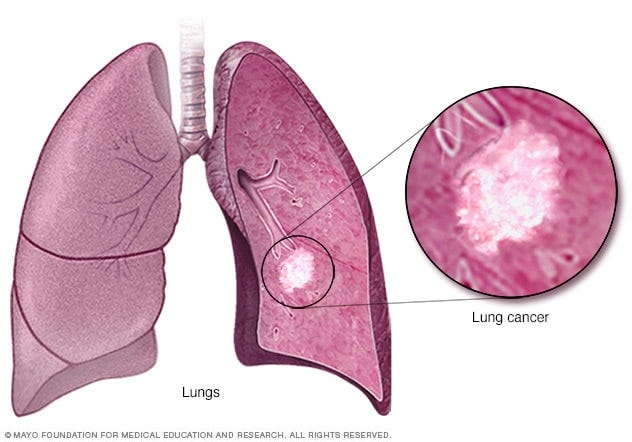
Tobacco smoke and smoking
Lung cancer is mostly brought on by tobacco smoke, a powerful carcinogen. The complex chemical mixture released when a person smokes tobacco damages lung tissue, causing genetic abnormalities and malignant growths. The length and frequency of smoking are directly correlated with the chance of acquiring lung cancer. Lung cancer risk is also increased by exposure to secondhand smoke. Smoking cessation greatly lowers the risk, but the long-lasting consequences of earlier smoking highlight the urgent need for public health initiatives that support early detection and prevention measures.
Environmental and occupational exposures
1. Radon gas
Radon gas, a colorless and odorless radioactive element, can accumulate in buildings and increase lung cancer risk upon inhalation. It originates from soil and rock and is the second leading cause of lung cancer after smoking. Reduce exposure and associated health risks by using proper ventilation and radon testing.
2. Asbestos
Due to its fire-retardant qualities, the group of naturally occurring minerals known as asbestos has been extensively exploited in industry and building. On the other hand, inhaling asbestos fibers can cause mesothelioma, asbestosis, and lung cancer. These tiny threads penetrate lung tissue after inhalation and cause genetic harm and inflammation. To limit additional exposure and the resulting health concerns, strict occupational and environmental laws are crucial.
3. Air pollution
Lung cancer is significantly increased by air pollution, which is a mixture of hazardous particles and gases from numerous sources. Nitrogen dioxide and benzene are two harmful gases that can irritate the respiratory system, causing persistent inflammation, DNA damage, and the emergence of cancer. Urban areas with high traffic and industrial emissions are particularly vulnerable. Lung cancer incidence must be reduced by the implementation of sustainable practices and changes to policy.
Genetic and familial predisposition
Lung cancer susceptibility is influenced by genetic and family variables. Lung cancer risk can be raised by inherited genetic mutations, such as those in the EGFR, KRAS, and TP53 genes. Moreover, a family history of lung cancer can indicate shared genetic susceptibility or common environmental exposures. These mutations can be found by genetic testing, which can also help with treatment selection. In order to identify high-risk individuals and advance precision medicine techniques for lung cancer prevention, early detection, and management, it is crucial to comprehend how genetics and environmental variables interact.
Pathogenesis and Molecular Mechanisms
Intricate molecular mechanisms driven by genetic changes and signaling pathways play a crucial role in the pathogenesis of lung cancer. Mutations in tumor suppressor genes like TP53 and oncogenes like EGFR and ALK impair normal cellular processes, encouraging unchecked growth and cell death evasion. Dysregulated pathways like the PI3K-AKT-mTOR and MAPK pathways further amplify tumor progression. Immune responses against cancer cells are hampered by immune evasion mechanisms including PD-L1 expression. Emerging targeted therapies and immunotherapies exploit these molecular aberrations to halt tumor growth and enhance immune recognition. A thorough comprehension of these complex networks holds promise for more efficient and individualized lung cancer treatments.
Clinical Presentation and Diagnosis
Lung cancer’s clinical appearance can range from mild symptoms like a persistent cough, shortness of breath, and chest pain to more obvious signs like weight loss and hemoptysis that indicate an advanced stage of the disease. Early diagnosis is challenging due to non-specific symptoms. Imaging methods including X-rays, CT scans, and PET scans are diagnostic tools that can be used to determine the size and spread of tumors. Cancer type and stage are confirmed by biopsies. Staging, often using TNM classification, determines disease extent. Improved imaging technologies and early detection programs help diagnose lung cancer earlier, allowing for more efficient treatment plans and perhaps better outcomes.
Treatment Options
Surgery
When treating lung cancer, especially in localized cases, surgery is essential. Procedures like lobectomy, pneumonectomy, and wedge resection involve removing affected lung tissue. Video-assisted thoracoscopic surgery (VATS), among other minimally invasive procedures, has improved patient recovery and cut down on hospital stays. Proper hospital management ensures preoperative assessment, skilled surgical teams, and postoperative care. Improved patient outcomes in the treatment of lung cancer result from surgical treatments combined with adjuvant medicines.
Radiation therapy
An essential component of the management of lung cancer is radiation therapy. It targets cancer cells with high-energy photons to prevent their division and proliferation. External beam radiation precisely directs radiation to the tumor site while sparing healthy tissues. This non-invasive approach is typically used in conjunction with chemotherapy or surgery to help shrink tumors, control local illness, and enhance the effectiveness of lung cancer treatment overall.
Chemotherapy
A key component of lung cancer treatment, chemotherapy involves the use of potent medications to kill rapidly dividing cancer cells. It targets cancer cells throughout the body and is given intravenously or orally to stop their proliferation. Platinum-based regimens are commonly employed, sometimes in combination with targeted therapies. Although there may be adverse effects from chemotherapy, improvements in supportive care lessen their severity. For patients with lung cancer, customized chemotherapy regimens help to enhance quality of life and survival.
Immunotherapy
Utilizing the immune system to specifically target and eradicate cancer cells, immunotherapy has revolutionized the way that lung cancer is treated. T cells may recognize and destroy cancer cells because checkpoint inhibitors, such as PD-1 and PD-L1 inhibitors, disrupt the proteins that suppress immune responses. Particularly when lung cancer is in its advanced stages, this strategy has demonstrated astounding success. Immunotherapy presents a promising approach for enhancing long-term outcomes and patient quality of life since it provides long-lasting advantages with tolerable adverse effects.
Targeted Therapies
Targeted medicines for the treatment of lung cancer concentrate on particular genetic abnormalities or tumor-promoting proteins. These medications have fewer side effects than conventional chemotherapy because they selectively target cancer cells while sparing healthy tissue. As examples, consider EGFR and ALK inhibitors for particular genetic mutations. Genetic testing-based precision medicine methods help identify potential patients for targeted medicines, improving results and allowing for more individualized lung cancer treatment.
Emerging and experimental treatments
Innovative tactics that push the limits of conventional therapy are a part of lung cancer’s experimental and emerging therapies. The goal of gene therapy is to stop the spread of cancer by altering the patient’s genes. CAR-T cell therapy engineers’ immune cells to target cancer cells. Cancer cells are infected and killed by oncolytic viruses. In-depth research is being done on these promising strategies, which could lead to healthcare management breakthroughs for lung cancer. Before they are widely used in healthcare, however, more research and clinical trials are required to determine their safety and effectiveness.
Prognosis and Survival Rates
The stage of lung cancer at diagnosis, the type of tumor, and the response to treatment are all important considerations. Due to late-stage diagnoses, lung cancer has a decreased overall survival rate. Small cell lung cancer (SCLC) and non-small cell lung cancer (NSCLC) both have higher overall survival rates. For certain patients, the results of targeted healthcare treatments and immunotherapy have improved. Early-stage detection significantly enhances prognosis, while advanced cases have a more guarded outlook. Collaboration between medical staff, patients, and support groups is essential for raising survival rates and ensuring the highest quality of life possible while battling lung cancer.
Prevention and Early Detection
Reducing exposure to risk factors including smoking and environmental toxins is a key step in preventing lung cancer. Campaigns and laws against smoking are essential parts of public health initiatives. A key factor in bettering outcomes is early detection. Hospital management should prioritize implementing screening programs, such as low-dose CT scans, for high-risk individuals. These programs provide early diagnosis during asymptomatic stages, improving the efficiency of treatment. A comprehensive strategy for prevention and early diagnosis can considerably lessen the impact of lung cancer on people and healthcare systems when combined with improvements in imaging technology, regular check-ups, and patient education.
Support and Palliative Care
Comprehensive lung cancer management includes support and palliative care as essential components. Throughout their journey, patients and their family get psychological, emotional, and informational assistance. By controlling symptoms like pain and dyspnea, minimizing treatment side effects, and addressing mental distress, palliative care aims to improve quality of life. The demands of patients’ physical, emotional, and spiritual well-being are satisfied thanks to this multidisciplinary approach. Hospice care provides comfort and dignity in advanced stages. Hospital administration should incorporate these programs into the continuum of treatment, providing patients with all-encompassing support so they may negotiate the difficulties of lung cancer with improved wellbeing and comprehension.
Ongoing Research and Future
Current research on lung cancer focuses on improving diagnosis, treatments, and comprehending fundamental causes. The identification of possible targets for individualized therapy is aided by genetic profiling, and immunotherapies are continuously improved. Gene editing and CAR-T cell therapy are two cutting-edge treatments that have the potential to completely change how lung cancer is managed. In order to provide seamless data sharing between healthcare practitioners, support real-time decision-making, patient monitoring, and collaborative research, the QMe Healthcare Management and Information System is essential to this advancement. Its inclusion in lung cancer research enables medical practitioners to provide state-of-the-art care and advance the field.
Conclusion
Finally, the complex terrain of lung cancer necessitates a diversified strategy. To effectively address this global health issue, healthcare professionals, researchers, and patients must work together on everything from prevention and early detection to individualized treatments and supportive care. In this process, the QMe Healthcare Management and Information System serves as a catalyst by facilitating communication, stimulating innovation, and improving data-driven decision-making. As strides in research continue, informed by robust data exchange and analysis, the horizon of lung cancer management brightens. Together, we strive for improved outcomes, extended survival, and enhanced quality of life for those affected by this complex disease.
- “Empowering Emergency Medicine Physicians”
- “Queue Management Software and Hospitalists in Modern Healthcare”
- “Enhancing-Pediatric-Infectious-Disease-Care”
- “Revolutionizing-Geriatric-Care”
- “Optimizing-Patient-Care-in-Pediatric-Rheumatology”
- “Pediatric-Pulmonology-Care”
- “Revolutionizing-Pediatric-Gastroenterology”
- “Enhancing-Pediatric-Neurology-Care”
- “Optimizing-Pediatric-Cardiology”
- “Enhancing-Pediatric-Endocrinology-Care”
- “Empowering-Neonatologists-with-EMR-Software”
- “Pediatrics-in-Focus”
- “Empowering-Neurologists-with-Electronic-Prescriptions”
- “Streamlining-Dermatology-Practice”
- “Streamlining-Psychiatry-Practice”
- “A-Game-Changer-for-Infectious-Disease-Specialists”
- “Allergist/Immunologist-Practices-with-QME-EMR-and-Hospital-Management-Systems”
- “Empowering-Hematologists-and-Revolutionizing-Healthcare-Management”
- “Optimizing-Healthcare-with-HMIS”
- “Transforming-Healthcare-with-Endocrinologist”
- “Healthcare-Management-with-QMe-EMR-for-Nephrologists”
- “Revolutionizing-Healthcare-Management-with-Cardiologist”
- “Streamlining-Operations-with-Queue-Management-Software”
- “Optimizing-Healthcare-Delivery”
- “Transforming-Healthcare-Management”
- HMIS And Decision Support Systems
- Dengue Unveiled: An Overview of Causes, Symptoms, and Prevention.
- Dengue Fever: Unraveling the Mosquito-Borne Menace.
- HMIS-and-Continuity-of-Care
- Project-Management-for-Successful-HMIS
- Catalysts of Wellness: The Transformative Power of Diagnosis and Screening in Healthcare
- Patient-Data-Management
- Guardians of Healthcare: The Vital Role of Fraud Detection in Ensuring Ethical Care
- Unlocking Insights
- Healthcare in the Digital Age: The History Of Development Of HMIS
- Transforming Healthcare
- Safeguarding-HMIS-Data
- HMIS-Integration-Challenges
- ANXIETY UNVEILED: CONQUERING FEARS AND CULTIVATING CALM.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- HMIS and Resource Allocation
- HMIS Data Accuracy and Integrity
- SOOTHING THE SILENT PAIN: UNDERSTANDING VULVODYNIA.
- Impact of HMIS on OPD Operations
- In Patient Management Through Health Management
- WITHIN THE SHADOWS: UNDERSTANDING BRAIN TUMOURS FROM WITHIN
- HMIS-and-Health-Insurance-Integration
- HMIS-Data-Analytics-for-Preventive-Care
- SILENT INTRUDERS: UNRAVELLING THE MYSTERIES OF PELVIC INFLAMMATORY DISEASE
- BREAKING FREE: OVERCOMING THE HURDLE OF URINARY INCONTINENCE
- “HMIS and Doctor-Patient Communication”
- HEALING INSIGHTS: THE POWER OF THE HOSPITAL MANAGEMENT INFORMATION SYSTEM.
- SOLVING THE OVARIAN PUZZLE:UNDERSTANDING OVARIAN CYST INSIDE OUT
- Usability And User Experience In HMIS
- WARRIOR’S BATTLE: TRIUMPHING OVER UTERINE CANCER
- POLYCYSTIC OVARY PUZZLE: UNRAVELLING THE ENIGMA OF PCOS
- Unlocking-the-Potential-of-HMIS-Data-for Medical-Research-and-Healthcare-Policy-Enhancement
- Feminine Health Unplugged: Empowering Women in Vaginal Infection Awareness
- Revitalizing Feminine Comfort: A Journey Through Vaginal Wellness.
- HMIS Vendor Selection Guide
- UNDERSTANDING FIBROIDS: NAVIGATING THE INTRICACIES OF UTERINE HEALTH.
- Best Practices for Data Migration in Healthcare Management Information Systems (HMIS)
- CONCEIVING HOPE: NAVIGATING THE JOURNEY OF INFERTILITY
- MENSTRUAL IRREGULARITIES: CAUSES AND TREATMENT
- RISING ABOVE: EMPOWERING WOMEN WITH PELVIC ORGAN PROLAPSE
- Leveraging HMIS for Enhanced Public Health Management and Disease Surveillance
- Challenges and Benefits of Implementing HMIS in Rural and Remote Healthcare Settings
- Securing Healthcare Continuity
- Pancreatic Cancer
- Lymphoma
- Leukemia
- Bladder Cancer
- Skin Cancer (Melanoma)
- COLORECTAL CANCER
- All about Prostate Cancer
- Advances in Breast Cancer Treatment: A Comprehensive Guide
- Autism Spectrum Disorder (ASD)
- EHR SYMPHONY: HARMONIZING HEALTHCARE THROUGH ELECTRONIC RECORDS .
- Understanding Testicular Cancer: Detection, Treatment And Awareness.
- Childhood Obesity
- Kawasaki Disease
- Eczema (Atopic Dermatitis)
- Understanding Bone Cancer: A Brief Overview.
- Virtual Healing: Navigating Healthcare Through Telemedicine and Telehealth.
- Attention-Deficit/Hyperactivity Disorder (ADHD)
- PELVIC PAIN:CAUSES SYMPTOMS AND PREVENTIONS
- Type 1 Diabetes: Causes, Symptoms, and Treatment
- Gastroesophageal Reflux Disease (GERD)
- Battling Pneumonia: Unveiling the Stealthy Invader of the Lungs
- Unravelling the Complexity of Allergic Reactions: Understanding, Managing, and Thriving
- Rashes (Eczema, Dermatitis)
- UNDERSTANDING CERVICAL DYSPLASIA: CAUSES, SYMPTOMS AND MANAGEMENT
- Chicken Pox
- Endometriosis Unmasked: A Closer Look at the Silent Struggle
- Croup
- Hand, Foot and Mouth Disease (HFMD)
- THE DAWNING OF A NEW ERA: EMBRACING THE JOURNEY OF MENOPAUSE
- Urinary Tract Infections (UTIs)
- Strep Throat (Streptococcal Pharyngitis)
- Understanding Otitis Media(Ear Infection)
- 28th July In medical history!!
- Influenza (Flu) - Symptoms, Prevention and Management
- 27th July In medical history!!
- Respiratory Syncytial Virus (RSV) Infection
- SIGNIFICANCE AND ADVANTAGES OF HMIS: A DETAILED ANALYSIS
- Beyond Boundaries: Transforming Healthcare with Virtual Reality
- TRACK YOUR LIFE : A DETAILED UNDERSTANDING ON HEALTH MONITORING SYSTEM
- EXPLORING BENEATH THE SURFACE: UNDERSTANDING BARTHOLIN CYSTS AND ABSCESSES
- GUARDING GUT HEALTH: YOUR GUIDE TO POTENTIAL CROHN’S DISEASE PREVENTION.
- PATHWAYS OF HOPE: NAVIGATING THE CHALLENGES OF ESOPHAGEAL CANCER
- Gastric Battles: Confronting Stomach Cancer Head-On.
- HMIS IN SMALL CLINICS: A STEP TO A BETTER FUTURE
- Harmonizing Your Cycle: A Journey to Menstrual Health and Balance.
- Respiratory Syncytial Virus (RSV) Infection
- GUARDING OUR INTIMATE WORLD: A CLOSER LOOK AT STI
- Real-World HMIS Implementation Case Studies: Using Data to Transform Healthcare
- Gastroenteritis (Stomach Flu)
- Asthama - The Anatomy Of Breathing
- Influenza - A Silent Intruder
- Breast Cancer