- “Empowering Emergency Medicine Physicians”
- “Queue Management Software and Hospitalists in Modern Healthcare”
- “Enhancing-Pediatric-Infectious-Disease-Care”
- “Revolutionizing-Geriatric-Care”
- “Optimizing-Patient-Care-in-Pediatric-Rheumatology”
- “Pediatric-Pulmonology-Care”
- “Revolutionizing-Pediatric-Gastroenterology”
- “Enhancing-Pediatric-Neurology-Care”
- “Optimizing-Pediatric-Cardiology”
- “Enhancing-Pediatric-Endocrinology-Care”
- “Empowering-Neonatologists-with-EMR-Software”
- “Pediatrics-in-Focus”
- “Empowering-Neurologists-with-Electronic-Prescriptions”
- “Streamlining-Dermatology-Practice”
- “Streamlining-Psychiatry-Practice”
- “A-Game-Changer-for-Infectious-Disease-Specialists”
- “Allergist/Immunologist-Practices-with-QME-EMR-and-Hospital-Management-Systems”
- “Empowering-Hematologists-and-Revolutionizing-Healthcare-Management”
- “Optimizing-Healthcare-with-HMIS”
- “Transforming-Healthcare-with-Endocrinologist”
- “Healthcare-Management-with-QMe-EMR-for-Nephrologists”
- “Revolutionizing-Healthcare-Management-with-Cardiologist”
- “Streamlining-Operations-with-Queue-Management-Software”
- “Optimizing-Healthcare-Delivery”
- “Transforming-Healthcare-Management”
- HMIS And Decision Support Systems
- Dengue Unveiled: An Overview of Causes, Symptoms, and Prevention.
- Dengue Fever: Unraveling the Mosquito-Borne Menace.
- HMIS-and-Continuity-of-Care
- Project-Management-for-Successful-HMIS
- Catalysts of Wellness: The Transformative Power of Diagnosis and Screening in Healthcare
- Patient-Data-Management
- Guardians of Healthcare: The Vital Role of Fraud Detection in Ensuring Ethical Care
- Unlocking Insights
- Healthcare in the Digital Age: The History Of Development Of HMIS
- Transforming Healthcare
- Safeguarding-HMIS-Data
- HMIS-Integration-Challenges
- ANXIETY UNVEILED: CONQUERING FEARS AND CULTIVATING CALM.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- HMIS and Resource Allocation
- HMIS Data Accuracy and Integrity
- SOOTHING THE SILENT PAIN: UNDERSTANDING VULVODYNIA.
- Impact of HMIS on OPD Operations
- In Patient Management Through Health Management
- WITHIN THE SHADOWS: UNDERSTANDING BRAIN TUMOURS FROM WITHIN
- HMIS-and-Health-Insurance-Integration
- HMIS-Data-Analytics-for-Preventive-Care
- SILENT INTRUDERS: UNRAVELLING THE MYSTERIES OF PELVIC INFLAMMATORY DISEASE
- BREAKING FREE: OVERCOMING THE HURDLE OF URINARY INCONTINENCE
- “HMIS and Doctor-Patient Communication”
- HEALING INSIGHTS: THE POWER OF THE HOSPITAL MANAGEMENT INFORMATION SYSTEM.
- SOLVING THE OVARIAN PUZZLE:UNDERSTANDING OVARIAN CYST INSIDE OUT
- Usability And User Experience In HMIS
- WARRIOR’S BATTLE: TRIUMPHING OVER UTERINE CANCER
- POLYCYSTIC OVARY PUZZLE: UNRAVELLING THE ENIGMA OF PCOS
- Unlocking-the-Potential-of-HMIS-Data-for Medical-Research-and-Healthcare-Policy-Enhancement
- Feminine Health Unplugged: Empowering Women in Vaginal Infection Awareness
- Revitalizing Feminine Comfort: A Journey Through Vaginal Wellness.
- HMIS Vendor Selection Guide
- UNDERSTANDING FIBROIDS: NAVIGATING THE INTRICACIES OF UTERINE HEALTH.
- Best Practices for Data Migration in Healthcare Management Information Systems (HMIS)
- CONCEIVING HOPE: NAVIGATING THE JOURNEY OF INFERTILITY
- MENSTRUAL IRREGULARITIES: CAUSES AND TREATMENT
- RISING ABOVE: EMPOWERING WOMEN WITH PELVIC ORGAN PROLAPSE
- Leveraging HMIS for Enhanced Public Health Management and Disease Surveillance
- Challenges and Benefits of Implementing HMIS in Rural and Remote Healthcare Settings
- Securing Healthcare Continuity
- Pancreatic Cancer
- Lymphoma
- Leukemia
- Bladder Cancer
- Skin Cancer (Melanoma)
- COLORECTAL CANCER
- All about Prostate Cancer
- Fighting out the Disease of Lung Cancer
- Advances in Breast Cancer Treatment: A Comprehensive Guide
- Autism Spectrum Disorder (ASD)
- EHR SYMPHONY: HARMONIZING HEALTHCARE THROUGH ELECTRONIC RECORDS .
- Understanding Testicular Cancer: Detection, Treatment And Awareness.
- Childhood Obesity
- Eczema (Atopic Dermatitis)
- Understanding Bone Cancer: A Brief Overview.
- Virtual Healing: Navigating Healthcare Through Telemedicine and Telehealth.
- Attention-Deficit/Hyperactivity Disorder (ADHD)
- PELVIC PAIN:CAUSES SYMPTOMS AND PREVENTIONS
- Type 1 Diabetes: Causes, Symptoms, and Treatment
- Gastroesophageal Reflux Disease (GERD)
- Battling Pneumonia: Unveiling the Stealthy Invader of the Lungs
- Unravelling the Complexity of Allergic Reactions: Understanding, Managing, and Thriving
- Rashes (Eczema, Dermatitis)
- UNDERSTANDING CERVICAL DYSPLASIA: CAUSES, SYMPTOMS AND MANAGEMENT
- Chicken Pox
- Endometriosis Unmasked: A Closer Look at the Silent Struggle
- Croup
- Hand, Foot and Mouth Disease (HFMD)
- THE DAWNING OF A NEW ERA: EMBRACING THE JOURNEY OF MENOPAUSE
- Urinary Tract Infections (UTIs)
- Strep Throat (Streptococcal Pharyngitis)
- Understanding Otitis Media(Ear Infection)
- 28th July In medical history!!
- Influenza (Flu) - Symptoms, Prevention and Management
- 27th July In medical history!!
- Respiratory Syncytial Virus (RSV) Infection
- SIGNIFICANCE AND ADVANTAGES OF HMIS: A DETAILED ANALYSIS
- Beyond Boundaries: Transforming Healthcare with Virtual Reality
- TRACK YOUR LIFE : A DETAILED UNDERSTANDING ON HEALTH MONITORING SYSTEM
- EXPLORING BENEATH THE SURFACE: UNDERSTANDING BARTHOLIN CYSTS AND ABSCESSES
- GUARDING GUT HEALTH: YOUR GUIDE TO POTENTIAL CROHN’S DISEASE PREVENTION.
- PATHWAYS OF HOPE: NAVIGATING THE CHALLENGES OF ESOPHAGEAL CANCER
- Gastric Battles: Confronting Stomach Cancer Head-On.
- HMIS IN SMALL CLINICS: A STEP TO A BETTER FUTURE
- Harmonizing Your Cycle: A Journey to Menstrual Health and Balance.
- Respiratory Syncytial Virus (RSV) Infection
- GUARDING OUR INTIMATE WORLD: A CLOSER LOOK AT STI
- Real-World HMIS Implementation Case Studies: Using Data to Transform Healthcare
- Gastroenteritis (Stomach Flu)
- Asthama - The Anatomy Of Breathing
- Influenza - A Silent Intruder
- Breast Cancer
Kawasaki Disease
Symptoms, Causes, Diagnosis, and Treatment of Kawasaki Disease
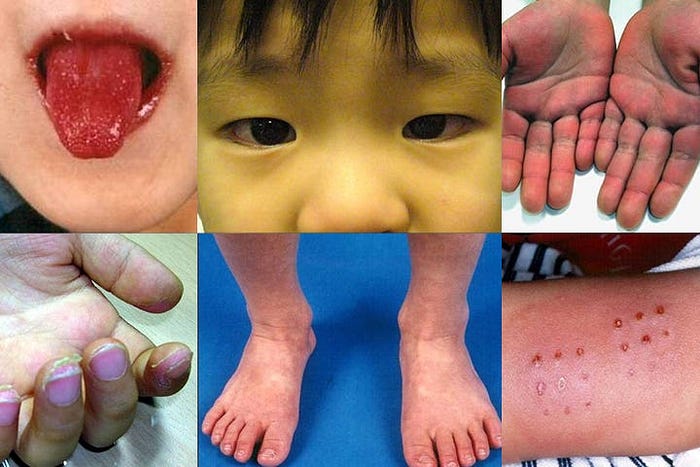
A rare but potentially dangerous juvenile ailment known as Kawasaki Disease (KD) predominantly affects blood vessels throughout the body. Characterized by fever, skin rash, and inflammation, KD can lead to complications, particularly involving the heart. Despite its rarity, KD needs to be taken seriously because it can lead to long-term cardiovascular problems and damage to the coronary arteries. For early intervention and better results, it is essential to comprehend the disease’s symptoms, causes, diagnosis, and therapy. The complexity of KD is examined in this article, along with its clinical manifestation, diagnostic techniques, existing treatments, and ongoing research projects aimed at improving our knowledge of and ability to treat this disorder.
What is Kawasaki Disease?
Kawasaki Disease (KD) is a rare pediatric vasculitis that typically affects children under the age of five and causes blood vessel inflammation. Marked by persistent high fever, it leads to various symptoms including red eyes, rash, swollen lymph nodes, and swollen hands or feet. KD can have major effects, namely coronary artery aneurysms that may cause cardiac problems. Although the precise etiology is still unknown, early identification and treatment, typically comprising intravenous immunoglobulin therapy and aspirin, are crucial for reducing the severity of the illness. For a good prognosis and long-term wellbeing, prompt recognition and management are essential.
Symptoms and Clinical Presentation
The symptoms of Kawasaki disease, which primarily affects children under the age of five, include a prolonged fever, red eyes, rash, swollen lymph nodes, and swollen extremities. Less common symptoms include cardiovascular involvement and vasculitis. Due to the possibility of issues with the coronary arteries, an early diagnosis is essential. Understanding the wide spectrum of symptoms and how they develop helps with appropriate management and quick medical intervention.
Epidemiology and Demographics

Kawasaki Disease exhibits a bimodal age distribution, predominantly striking children under five years old and, to a lesser extent, individuals aged 5–10. Asian populations, particularly those in Japan, Korea, and Taiwan, have a higher incidence of it. While the disease affects both genders, it’s slightly more common in boys. Geographically, variations exist, with higher prevalence in Asian countries, followed by lower but increasing rates in North America and Europe. Uncertainty over the causes of these demographic patterns points to a complicated interplay between genetic predisposition and environmental influences. For more effective clinical management and targeted awareness campaigns, a thorough understanding of these patterns is necessary.
Causes and Risk Factors
The exact cause of Kawasaki Disease (KD) remains elusive, but a combination of genetic susceptibility and environmental triggers is likely. The illness could be caused by an overreacting immune system to a virus or other infectious factor. Genetic factors influence susceptibility, as KD tends to occur more frequently in families with a history of the disease. A further factor is ethnicity, with Asian populations experiencing greater rates. Some environmental elements, such as poisons or pollutants, may play a role in the development of disease. It is imperative to gather more knowledge about these causes and risk factors in order to improve KD early detection, treatment, and perhaps even the creation of preventative strategies.
Diagnosis and Differential Diagnosis

Diagnosing Kawasaki Disease (KD) relies on clinical criteria, requiring persistent fever along with specific symptoms like rash, conjunctivitis, and swollen lymph nodes. Since these symptoms can mimic other illnesses, a thorough differential diagnosis is crucial to exclude similar conditions such as scarlet fever, toxic shock syndrome, and viral infections. Echocardiography is a type of diagnostic imaging that aids in determining cardiac involvement. Priority should be given to early diagnosis because timely treatment lowers the likelihood of complications. Healthcare personnel must be acutely aware of KD’s clinical presentation and use precise diagnostic techniques given the risk of coronary artery aneurysms in order to ensure accurate and prompt intervention.
Medical Evaluation and Tests
A thorough physical examination is necessary for the medical evaluation of Kawasaki disease in order to spot important signs and symptoms such fever, rash, and conjunctivitis. Blood tests are useful for identifying inflammatory indicators and excluding other diseases. In order to identify potential heart problems such anomalies in the coronary arteries, echocardiography is essential. Clinicians also evaluate the patient’s medical background and take into account the persistence and evolution of symptoms. For a precise diagnosis and prompt treatment, a multidisciplinary strategy comprising pediatricians, cardiologists, and rheumatologists is necessary.
Treatment and Management

Treatment of Kawasaki Disease involves hospitalization for close monitoring. The primary approach includes administering intravenous immunoglobulin (IVIG) therapy to reduce inflammation and fever. Additionally, aspirin medication is recommended to ease symptoms and lower the chance of blood clots. It is crucial to provide close aftercare and watch for any potential problems, especially cardiac ones. Effective healthcare management is ensured through cooperation between pediatricians, cardiologists, and other specialists. Early management is crucial for improving the general prognosis and wellbeing of Kawasaki Disease patients since it dramatically lowers the risk of coronary artery problems.
Long-Term Effects and Complications
The possibility of coronary artery anomalies, which can result in heart issues like myocardial infarction or heart failure, is one of Kawasaki Disease’s long-term repercussions. Coronary artery aneurysms may develop in untreated or severe cases, necessitating potential lifelong monitoring and hospital treatment. Additionally, there may be a connection between Kawasaki disease and adult cardiovascular problems. Neurological and developmental concerns, although less common, have also been reported. The significance of continued medical surveillance, even after the acute stage of the disease, to enable early detection and effective care of any emergent difficulties is highlighted by an understanding of these potential complications.
Prognosis and Outlook
With timely and effective treatment, the prognosis for Kawasaki Disease (KD) is generally favorable. Early intervention, especially within the first ten days of fever onset, significantly reduces the risk of coronary artery abnormalities and associated complications. The majority of children recover fully without long-term issues. The severity of coronary involvement and the patient’s reaction to treatment are two variables that can affect the result. To check for any potential heart-related problems, it is essential to have regular cardiac follow-ups. The prognosis for affected children keeps getting better as medical knowledge of KD advances, along with increasing awareness and prompt medical intervention.
Research and Advancements
Uncovering the precise causes and underlying mechanisms of Kawasaki Disease (KD), including the potential contributions of genetics and immunological responses, is the subject of ongoing research. Biomarkers and genetic testing are two examples of diagnostic tool improvements that attempt to increase early detection and expand healthcare treatment options. To further improve results, lower inflammation, and avoid problems such coronary artery aneurysms, innovative medicines are also being investigated. The possibility of preventive measures in the future is being opened up through international collaborations between academics, doctors, and institutions that are paving the way for a deeper understanding of KD.
By gathering patient data, supporting clinical trials, and enabling real-time monitoring for conditions like Kawasaki Disease, QMe Hospital Management and Information System (HMIS) contribute to research and breakthroughs. HMIS encourages collaboration and data exchange while supporting decisions based on facts, quality enhancement, and long-term studies. Early detection is assisted by predictive analytics, and efficient care distribution is ensured through resource management. HMIS also improves healthcare personnel’ education, which benefits patients by improving outcomes and illness comprehension.
Prevention and Public Awareness
Raising public knowledge of Kawasaki disease (KD) symptoms, early intervention, and risk factors is essential to its prevention. It is crucial to run educational efforts aimed at parents, carers, and medical professionals. Encourage prompt medical attention by raising awareness of KD’s specific symptoms, which include a prolonged fever and rash. The necessity of early treatment is emphasized by distributing information about probable complications, particularly problems with the coronary arteries. By fostering a better understanding of KD’s characteristics and the significance of seeking medical care promptly, prevention efforts can lead to reduced morbidity and better long-term outcomes for affected children.
Conclusion
In summary, Kawasaki disease presents opportunities and difficulties for the field of pediatric health. For reducing potential consequences and guaranteeing the wellbeing of afflicted children, it is essential to recognize its complexity and receive a prompt diagnosis and good treatment. The future holds potential for better results with continuous study, medical improvements, and increasing public awareness.
QMe Hospital Management and Information System (HMIS) plays a pivotal role in this trajectory. The QMe HMIS supports collaborative efforts among healthcare professionals, research, and evidence-based decision-making by seamlessly integrating data collection, analysis, and patient management. Through real-time monitoring, predictive analytics, and resource optimization, it improves the standard of care. Additionally, QMe HMIS supports initiatives for education and awareness, enabling doctors to provide better care and families to seek immediate medical help. In this approach, QMe HMIS greatly enhances the lives of those who are impacted by this complex ailment by promoting the prevention, comprehension, and efficient management of Kawasaki Disease.
- “Empowering Emergency Medicine Physicians”
- “Queue Management Software and Hospitalists in Modern Healthcare”
- “Enhancing-Pediatric-Infectious-Disease-Care”
- “Revolutionizing-Geriatric-Care”
- “Optimizing-Patient-Care-in-Pediatric-Rheumatology”
- “Pediatric-Pulmonology-Care”
- “Revolutionizing-Pediatric-Gastroenterology”
- “Enhancing-Pediatric-Neurology-Care”
- “Optimizing-Pediatric-Cardiology”
- “Enhancing-Pediatric-Endocrinology-Care”
- “Empowering-Neonatologists-with-EMR-Software”
- “Pediatrics-in-Focus”
- “Empowering-Neurologists-with-Electronic-Prescriptions”
- “Streamlining-Dermatology-Practice”
- “Streamlining-Psychiatry-Practice”
- “A-Game-Changer-for-Infectious-Disease-Specialists”
- “Allergist/Immunologist-Practices-with-QME-EMR-and-Hospital-Management-Systems”
- “Empowering-Hematologists-and-Revolutionizing-Healthcare-Management”
- “Optimizing-Healthcare-with-HMIS”
- “Transforming-Healthcare-with-Endocrinologist”
- “Healthcare-Management-with-QMe-EMR-for-Nephrologists”
- “Revolutionizing-Healthcare-Management-with-Cardiologist”
- “Streamlining-Operations-with-Queue-Management-Software”
- “Optimizing-Healthcare-Delivery”
- “Transforming-Healthcare-Management”
- HMIS And Decision Support Systems
- Dengue Unveiled: An Overview of Causes, Symptoms, and Prevention.
- Dengue Fever: Unraveling the Mosquito-Borne Menace.
- HMIS-and-Continuity-of-Care
- Project-Management-for-Successful-HMIS
- Catalysts of Wellness: The Transformative Power of Diagnosis and Screening in Healthcare
- Patient-Data-Management
- Guardians of Healthcare: The Vital Role of Fraud Detection in Ensuring Ethical Care
- Unlocking Insights
- Healthcare in the Digital Age: The History Of Development Of HMIS
- Transforming Healthcare
- Safeguarding-HMIS-Data
- HMIS-Integration-Challenges
- ANXIETY UNVEILED: CONQUERING FEARS AND CULTIVATING CALM.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- BEYOND THE BLUE: EMBRACING LIGHT ON THE PATH OF DEPRESSION.
- HMIS and Resource Allocation
- HMIS Data Accuracy and Integrity
- SOOTHING THE SILENT PAIN: UNDERSTANDING VULVODYNIA.
- Impact of HMIS on OPD Operations
- In Patient Management Through Health Management
- WITHIN THE SHADOWS: UNDERSTANDING BRAIN TUMOURS FROM WITHIN
- HMIS-and-Health-Insurance-Integration
- HMIS-Data-Analytics-for-Preventive-Care
- SILENT INTRUDERS: UNRAVELLING THE MYSTERIES OF PELVIC INFLAMMATORY DISEASE
- BREAKING FREE: OVERCOMING THE HURDLE OF URINARY INCONTINENCE
- “HMIS and Doctor-Patient Communication”
- HEALING INSIGHTS: THE POWER OF THE HOSPITAL MANAGEMENT INFORMATION SYSTEM.
- SOLVING THE OVARIAN PUZZLE:UNDERSTANDING OVARIAN CYST INSIDE OUT
- Usability And User Experience In HMIS
- WARRIOR’S BATTLE: TRIUMPHING OVER UTERINE CANCER
- POLYCYSTIC OVARY PUZZLE: UNRAVELLING THE ENIGMA OF PCOS
- Unlocking-the-Potential-of-HMIS-Data-for Medical-Research-and-Healthcare-Policy-Enhancement
- Feminine Health Unplugged: Empowering Women in Vaginal Infection Awareness
- Revitalizing Feminine Comfort: A Journey Through Vaginal Wellness.
- HMIS Vendor Selection Guide
- UNDERSTANDING FIBROIDS: NAVIGATING THE INTRICACIES OF UTERINE HEALTH.
- Best Practices for Data Migration in Healthcare Management Information Systems (HMIS)
- CONCEIVING HOPE: NAVIGATING THE JOURNEY OF INFERTILITY
- MENSTRUAL IRREGULARITIES: CAUSES AND TREATMENT
- RISING ABOVE: EMPOWERING WOMEN WITH PELVIC ORGAN PROLAPSE
- Leveraging HMIS for Enhanced Public Health Management and Disease Surveillance
- Challenges and Benefits of Implementing HMIS in Rural and Remote Healthcare Settings
- Securing Healthcare Continuity
- Pancreatic Cancer
- Lymphoma
- Leukemia
- Bladder Cancer
- Skin Cancer (Melanoma)
- COLORECTAL CANCER
- All about Prostate Cancer
- Fighting out the Disease of Lung Cancer
- Advances in Breast Cancer Treatment: A Comprehensive Guide
- Autism Spectrum Disorder (ASD)
- EHR SYMPHONY: HARMONIZING HEALTHCARE THROUGH ELECTRONIC RECORDS .
- Understanding Testicular Cancer: Detection, Treatment And Awareness.
- Childhood Obesity
- Eczema (Atopic Dermatitis)
- Understanding Bone Cancer: A Brief Overview.
- Virtual Healing: Navigating Healthcare Through Telemedicine and Telehealth.
- Attention-Deficit/Hyperactivity Disorder (ADHD)
- PELVIC PAIN:CAUSES SYMPTOMS AND PREVENTIONS
- Type 1 Diabetes: Causes, Symptoms, and Treatment
- Gastroesophageal Reflux Disease (GERD)
- Battling Pneumonia: Unveiling the Stealthy Invader of the Lungs
- Unravelling the Complexity of Allergic Reactions: Understanding, Managing, and Thriving
- Rashes (Eczema, Dermatitis)
- UNDERSTANDING CERVICAL DYSPLASIA: CAUSES, SYMPTOMS AND MANAGEMENT
- Chicken Pox
- Endometriosis Unmasked: A Closer Look at the Silent Struggle
- Croup
- Hand, Foot and Mouth Disease (HFMD)
- THE DAWNING OF A NEW ERA: EMBRACING THE JOURNEY OF MENOPAUSE
- Urinary Tract Infections (UTIs)
- Strep Throat (Streptococcal Pharyngitis)
- Understanding Otitis Media(Ear Infection)
- 28th July In medical history!!
- Influenza (Flu) - Symptoms, Prevention and Management
- 27th July In medical history!!
- Respiratory Syncytial Virus (RSV) Infection
- SIGNIFICANCE AND ADVANTAGES OF HMIS: A DETAILED ANALYSIS
- Beyond Boundaries: Transforming Healthcare with Virtual Reality
- TRACK YOUR LIFE : A DETAILED UNDERSTANDING ON HEALTH MONITORING SYSTEM
- EXPLORING BENEATH THE SURFACE: UNDERSTANDING BARTHOLIN CYSTS AND ABSCESSES
- GUARDING GUT HEALTH: YOUR GUIDE TO POTENTIAL CROHN’S DISEASE PREVENTION.
- PATHWAYS OF HOPE: NAVIGATING THE CHALLENGES OF ESOPHAGEAL CANCER
- Gastric Battles: Confronting Stomach Cancer Head-On.
- HMIS IN SMALL CLINICS: A STEP TO A BETTER FUTURE
- Harmonizing Your Cycle: A Journey to Menstrual Health and Balance.
- Respiratory Syncytial Virus (RSV) Infection
- GUARDING OUR INTIMATE WORLD: A CLOSER LOOK AT STI
- Real-World HMIS Implementation Case Studies: Using Data to Transform Healthcare
- Gastroenteritis (Stomach Flu)
- Asthama - The Anatomy Of Breathing
- Influenza - A Silent Intruder
- Breast Cancer